While everyone may not know exactly what antibiotics are or how they work, most people have taken them at some point in their lives. Familiarity with antibiotics stems from the fact that they are prescribed often, and their frequency of misuse has led to a very big problem – antibiotic resistance. So what are we supposed to do when “take two of these and call me in the morning†stops working?
ESKAPE-ing the Resistance
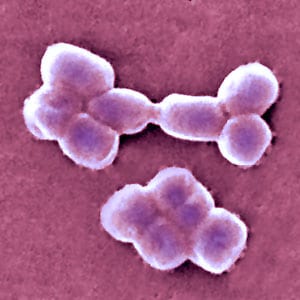
Recently, doctors at the University of California, San Diego (UCSD), in collaboration with research groups across the nation, raced the clock to save a man's life from a deadly, multi-drug resistant bacterial infection. Tom Patterson, a Ph.D. at the UCSD School of Medicine, contracted the infection and fell ill while on holiday in Egypt. When his symptoms – abdominal pain, nausea, fever – grew too severe, he was medically evacuated to Germany. After testing fluid surrounding a large cyst in his abdomen, an infection from the multi-drug resistant bacteria Acinetobacter baumannii was found. A. Baumannii is one of six types bacteria, known by the acronym ESKAPE, that are notorious for “escaping†death by common antibiotics. When Patterson was transferred to the ICU at UCSD Health, the doctors determined that the bacteria had become resistant to all the antibiotics he had been treated with. The situation managed to take a turn for the worst – Patterson's antibiotic-resistant bacterial infection became septic. He now had a life-threatening infection throughout his whole body.
Patterson's wife, Steffanie Strathdee, is also a Ph.D. and Chief of the Division of Global Public Health in the Department of Medicine at UCSD. With her husband now in a coma and facing certain death, she was forced to make drastic decisions for the sake of his life. She researched alternative therapies, reached out to scientific researchers, and worked with doctors to get emergency Food and Drug Administration (FDA) approval to try to treat her husband's infection with bacteriophages.
Bacterio-whats?! And how are they going to save this man's life?!
Simply put, Bacteriophages – also just called phages – are viruses that infect bacteria. Researchers are finding ways to utilize these viruses to fight bacterial infections, aka phage therapy! But phage therapy isn't actually a new idea. Knowledge of phages has been around for over a century, and phages were studied as a method of treatment prior to the advent of antibiotics in 1928. It's popularity waned since then, but with the rise of antibiotic resistance, there's a lot of revived interest.
Phage strains are very specific to the bacteria they target. This specificity poses a challenge to utilizing phages as a general course of treatment for bacterial infections because you need to know the type of bacteria in order to treat it. For Patterson's case, his doctors had to get emergency FDA approval for 3 specific types of phage. He came out of his coma a few days after the introduction of the phage therapy and returned home after a couple more months in the hospital. After the successful treatment of Patterson's and two other patients' infections, UCSD is opening the first Phage Therapy Center in the US.
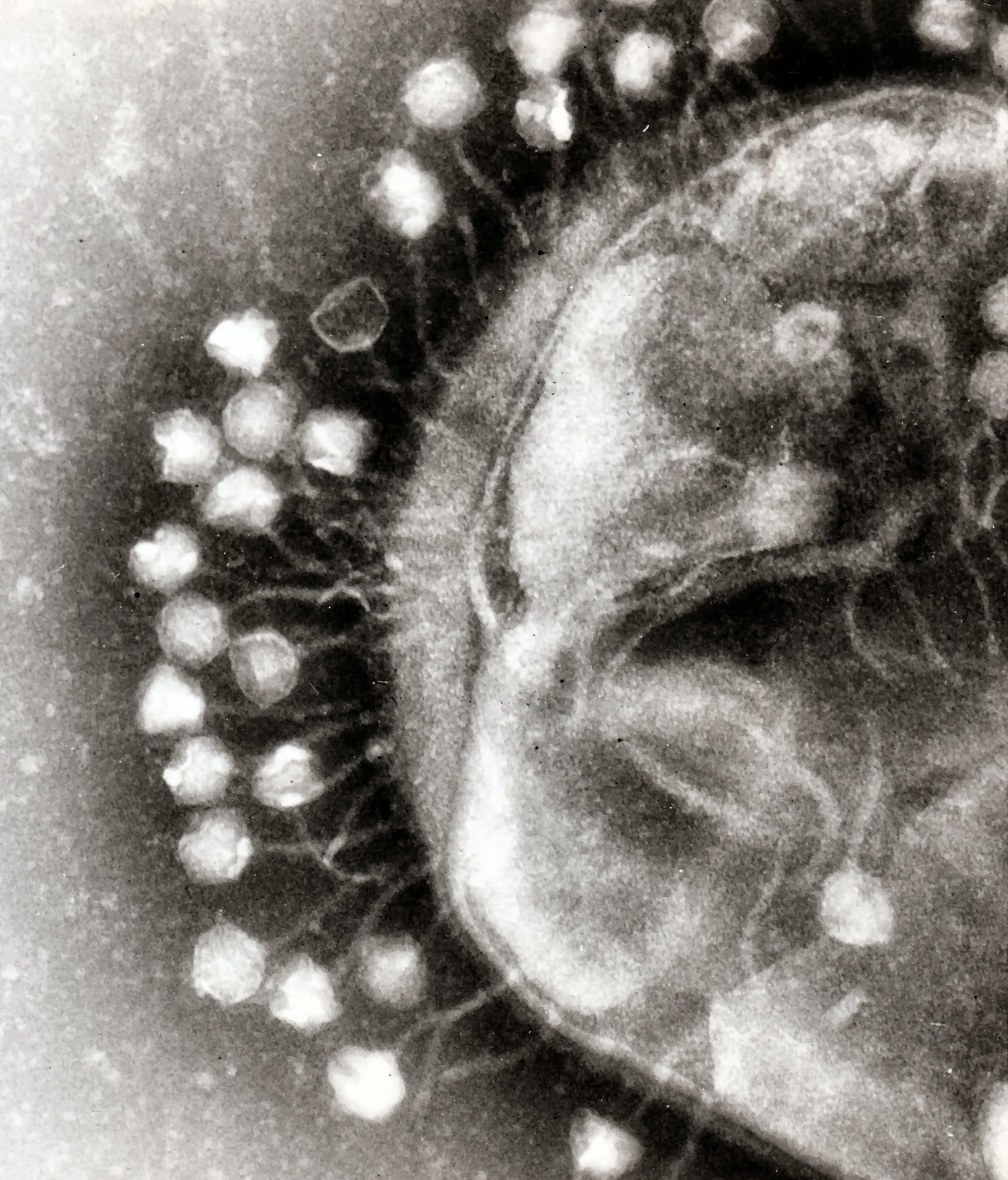
The enemy of my enemy can be my friend – turning phage into therapy.
Future medical cases from different bacteria than Patterson's would need approval for different phages; this creates a bit of a regulatory nightmare. The FDA will need to sort out how to handle approval and regulation for different phages to be used for different infections – there are approximately 1031 phage entities out there (a number higher than all other organisms on Earth combined), so it's no easy task! Also, as phages are being identified and characterized, doctors need to know which phage attack which bacteria, so that they can prescribe the right phage therapy. Researchers are already tackling the latter problem by establishing a Phage Directory. This will help keep track of which phages are characterized, and who has which phage species available for research or possible medical use.
With the threat of a post-antibiotic world looming, any step in the direction of new treatments can be a game-changer The handful of successful phage therapy cases in the US are certainly promising. The FDA could possibly take a page from Belgium's book, which recently became the first western nation to allow hospital pharmacists to regularly administer phage as a form of treatment after a doctor prescribes it. Perhaps this kind of regulation will provide useful guidance on how to incorporate phage therapy into modern medicine – helping to tackle the antibiotic resistance problem and changing the story of “take two of these†for future generations to come.
Featured image credit: 46137 via Flickr
 Michelle Dookwah is a graduate student at the University of Georgia Complex Carbohydrate Research Center, where she studies rare neurological disorders using patient stem cells. She's pretty passionate about science and science communication. However, she also enjoys numerous activities in her free time, including reading, listening to podcasts and audiobooks, hiking, baking, and obsessing over her labradoodle named Goose! More from Michelle Dookwah.
Michelle Dookwah is a graduate student at the University of Georgia Complex Carbohydrate Research Center, where she studies rare neurological disorders using patient stem cells. She's pretty passionate about science and science communication. However, she also enjoys numerous activities in her free time, including reading, listening to podcasts and audiobooks, hiking, baking, and obsessing over her labradoodle named Goose! More from Michelle Dookwah.
About the Author
-
athenssciencecafehttps://athensscienceobserver.com/author/athenssciencecafe/April 17, 2020
-
athenssciencecafehttps://athensscienceobserver.com/author/athenssciencecafe/April 12, 2020
-
athenssciencecafehttps://athensscienceobserver.com/author/athenssciencecafe/April 3, 2020
-
athenssciencecafehttps://athensscienceobserver.com/author/athenssciencecafe/March 30, 2020







