There is a mental health crisis in the STEM graduate community.
In this series, “Mental Wellness,†we will highlight not only the mental state of graduate students all over the world, but also the likely causes for these conditions, how to know when what you're feeling is too much, and how to deal with it in a healthy manner. So, take this journey with us and learn how to navigate grad school with a clean bill of mental health.
In modern day society, mental illness is still perceived as weakness. Just the words “mental health†can elicit a negative response and are frequently associated with hurtful words such as “freak†or “crazy.†Part of this stigma associated with mental illness is due to a lack of understanding of what these conditions actually are and why they are occurring. Depression, anxiety, stress, even schizophrenia and ADHD are behaviors which manifest due to real biological and biochemical responses happening in your brain. Here we will discuss exactly what occurs in your brain when feeling stressed, depressed, or anxious and how some common therapies change these processes.
The Everyday Brain
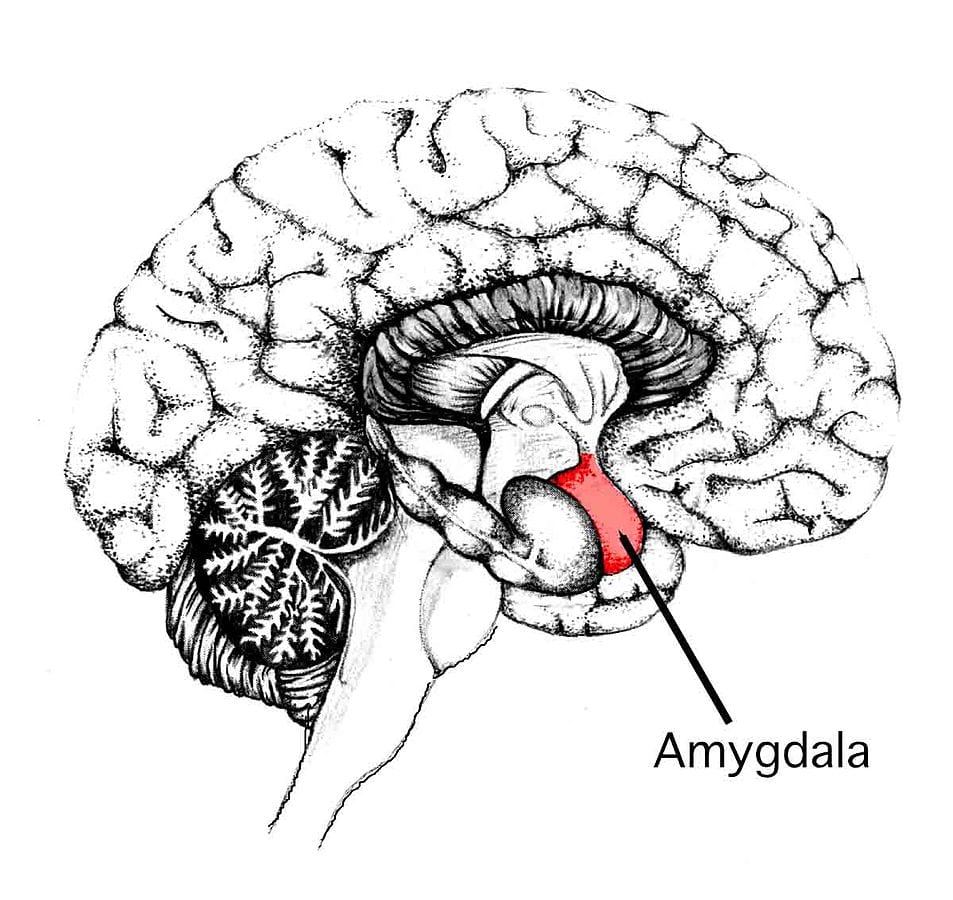
To understand the underlying biochemical processes associated with stress, anxiety, and depression we must first understand how our brains function in their absence. Within our brain is a small almond-shaped structure called the amygdala, which processes and interprets incoming sensory signals (sights, sounds, etc.). If a potential threat is detected it alerts the rest of the brain, mounting what is known as the “fight-or-flight†response. When you feel threatened, your heart rate accelerates, your breathing increases, you may even feel a heightened awareness of your surroundings. All of this prepares your body to either fight for your life or flee. This response is a good thing. It's our survival instinct. However, bad things can happen if this response is not properly regulated.

The Stressed Brain
Given what we know about the “fight-or-flight†response, it should be no surprise that stressful events also elicit this response. This is accompanied by signals from the brain which trigger the release of cortisol from the adrenal glands. Cortisol (aka the stress hormone) works within certain parts of the brain to control mood, motivation, and even fear. When the “fight-or-flight†response abates, cortisol levels, as well as heart rate and oxygen intake, return to normal. However, if the response is not resolved, cortisol can accumulate and derail many important bodily functions, as well as contribute to conditions including depression and anxiety.
The Anxious Brain
Anxiety is distinct from stress in that it manifests as fear or apprehension, something you may have experienced when taking an exam or speaking in public. While fear is typically a physical response to danger, anxiety is a psychological response to a perceived danger, even when there is no imminent threat. When giving a presentation, the audience isn't actually threatening you, but you may still fear speaking in public. Anything that evokes a negative emotion can trigger anxiety, and if you develop thinking patterns which reinforce these events as threatening, it can create a never-ending cycle of fear. Your body can become wired to search for potential threats, maintaining a constant state of “fight-or-flight†which can, in the most severe cases, trigger panic attacks and even panic disorders.

The Depressed Brain
While stress can also trigger depression, the biological basis of depression is much more complex. Although there are links between depression and elevated cortisol levels, much of what is known about the biology of depression has to do with the neurotransmitter serotonin, which regulates many important physiological processes including sleep, appetite, and mood. While many studies suggest that low levels of serotonin may be linked with depression, the biology of depression remains a mystery. However, given that many of the symptoms of depression are associated with serotonin, it is plausible that it may play a key role in regulating this process.
The Merits of Medication and Meditation
Research about these conditions suggests they are triggered by chemical imbalances within the brain, thus remedies (both natural and pharmaceutical) seek to rectify this. Popular medications include selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) which alter the amounts of serotonin and norepinephrine within the brain, boosting your mood and energy levels. Additionally, self-care activities such as exercise, meditation, and yoga can aid in reducing feelings of depression or anxiety. These activities not only provide an outlet for excess cortisol but also trigger the release of endorphins, chemicals which elevate your mood naturally.
So while people may say you’re “crazy†for feeling these things, it's important to understand that this is not the case. There is a reason for why you feel the way you do. But understanding the basis of these conditions is only half the battle – now what can we do to fix it? Stay tuned for the next post in my series, which will discuss ways to relieve the current mental health crisis.
For 24-hour assistance with problems related to mental health, please contact the Georgia Crisis and Access Line at (1-800-715-4225) or online at www.mygcal.com.
About the Author
 |
Katie Reagin is a Ph.D. Student in the Department of Cellular Biology at the University of Georgia, where she studies the immune response to influenza and other respiratory infections. When she is not in lab you can find her reading, painting, binge-watching Gilmore Girls, and pretending to be a food network chef in her kitchen. More from Katie Reagin. |







