Ladies, how many times have you rolled your eyes while your male friend languishes on the couch, suffering from a serious case of the “man flu†while the rest of us manage to take a decongestant and go about our day? Fellas, does it ever seem like every woman you know is constantly complaining of migraines? Well, what if this isn't all in our heads?
Although we often assume that our opposite-sex counterparts experience health and illness the same way we do, medical science says this is not always the case. However, basic and clinical research has not always been conducted in an all-inclusive manner, leading to widespread biases in our medical knowledge. While we are shifting away from this paradigm, it has no doubt contributed to a pattern of suboptimal care and missed diagnoses for many patients throughout the decades, particularly for women.
What makes us different?
Let's start with the obvious: females and males have physical differences in terms of sex organs and a myriad of secondary sex characteristics such as facial hair or breasts. In addition, the two sexes differ on a cellular and molecular level in ways that are invisible to the naked eye. In humans, every cell that makes up the female body contains two X chromosomes, while all male cells carry one X and one Y chromosome (the exception in each case being germ cells). These chromosomes carry different sets of genes, so to some extent, males and females are “coded†differently. Females also undergo regular and substantial fluctuations in their hormones throughout their fertility cycle, which males do not experience.
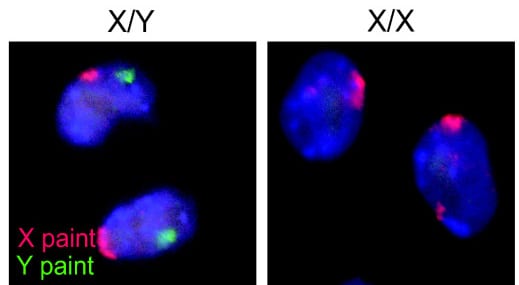
Until recently, it was assumed that these differences were only relevant in the context of reproduction, their scope limited to sex-specific disorders such as endometriosis or prostate cancer. For scientists trying to study heart disease, a female heart functions the same as a male heart, so why would it matter which one they used as a test subject?
Gender bias in research
Indeed, medical research has routinely been conducted using mostly male subjects, whether lab animal or human. Male subjects were considered to be more “controlledâ€; females were supposedly more confounding as a consequence of their hormones. The underlying assumption was that the data gathered from males would apply to females anyway. As such, females were underrepresented, if not outright excluded, in medical studies and clinical trials.
We now know that this assumption is fundamentally flawed. It turns out that a homogenous group of males does not make a good proxy for the entire population. An often cited example involves Ambien, a prescription sleep aid. For 20 years, it was universally prescribed using the guidelines that were established during trials that skewed heavily male. After two decades of complaints from women about lingering next-day impairment, evidence emerged that Ambien is actually metabolized more slowly in the female body. The recommended dosage has since been cut in half for female patients.

Incidence of disease
It's not just the way we respond to drugs; our different physiologies also play a role in how we experience illness. For instance, there is evidence that men have weaker immune systems than women, so not only are men more susceptible to infection, they also experience symptoms with greater severity and take longer to recover. However, there is a tradeoff; women are at far greater risk of developing autoimmune disorders, which cause a person’s immune system to become overactive and attack their own body.
As these discrepancies become more widely observed, many scientists are working to develop standards of best practice for including sex as a relevant factor in the study of disease models, epidemiology, and medical interventions. Despite these efforts, as of 2012, it was found that 22% of animal-based research studies published across five major surgical journals did not report sex at all, and of those that did, 80% still used exclusively male subjects.
Bridging the gaps
Fortunately, progress is being made. In 1993, the National Institutes of Health mandated that women must be included in all government funded health research. Between 2010 and 2012, an average of 43% of clinical trial participants for newly approved drugs were female, up from less than 20% in the 90s. For the first time in modern medicine, we are becoming sensitive to the differences in men's and women's health. But after over a century of downplaying these inconsistencies, we have a lot of catching up to do. In the meantime, maybe we can have a little more sympathy this man-cold and flu season.
About the Author
 |
Jennifer Kurasz is a graduate student in the Department of Microbiology at UGA, where she studies the regulation of RNA repair mechanisms in Salmonella. When not in the lab, she prefers to be mediocre at many hobbies rather than settle on one. She greatly enjoys her women's weightlifting group, cooking, painting, meditation, craft beer, and any activity that gets her outdoors. She can be contacted at jennifer.kurasz25@uga.edu. More from Jennifer Kurasz. |







