Header Image Courtesy of Flikr
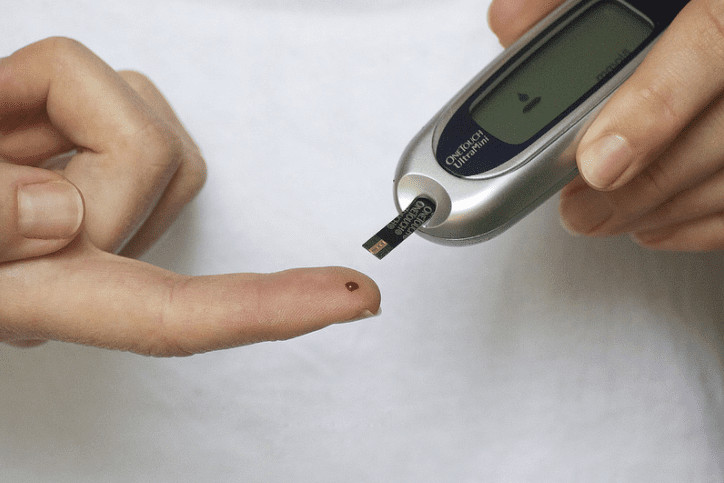
You wake up, and the first thing you think about is diabetes because you have to check your blood sugar … and kind of know where to start your day.
She was sitting in her kitchen, chatting over FaceTime as if a friend had just dropped by for a visit. It was Sunday night, and Meagan Sheikh and her husband were enjoying a few quiet hours after their young son went to sleep.
A hardworking wife and mother with a love for nursing, Meagan was diagnosed with Type I diabetes at the age of 26. Over time, Meagan has learned to balance her family, work life, and fluctuating blood sugar, all while sharing her experiences with others in her blog.
Meagan is one of approximately 29.1 million Americans currently living with a form of diabetes. Just like Meagan, every person has a unique experience with this complex disease.
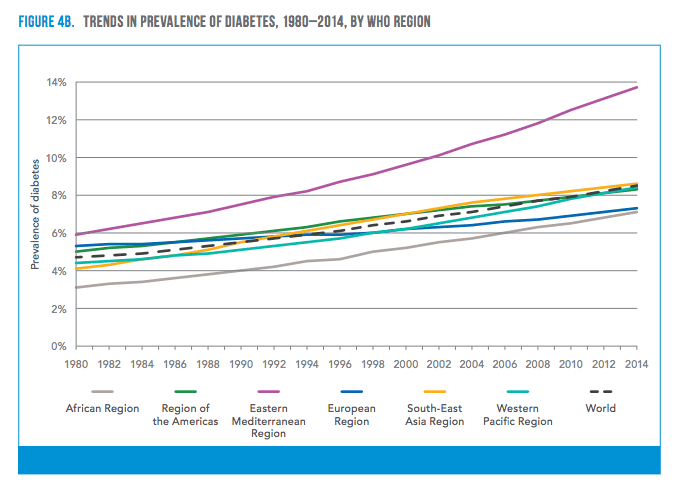
The World Health Organization recently published the Global Report on Diabetes to address the rising prevalence of diabetes across the globe. From 1980 until 2014, the number of people living with some form of diabetes nearly quadrupled from 108 million to 422 million. 1 in 20 people worldwide already have some form of diabetes, and those numbers are expected to climb rapidly. If current trends for Type II diabetes continue, 1 in 3 US citizens will be diagnosed in their lifetime.
What is diabetes?
The World Health Organization (WHO) describes diabetes as a “chronic, progressive disease characterized by elevated levels of blood glucose.†If that definition sounds broad to you, that's because it is. Diabetes is a general term for a family of diseases that occur for different reasons at different stages of life. The two most common varieties are Type I and Type II:
‣ Meagan was diagnosed with Type I at age 26 after having her first baby.
‣ Beth,* wife and mother of four, was diagnosed with Type II at 37.
‣ Anna, my friend and fellow UGA student, was diagnosed with Type I at 18.
*This name has been changed to protect privacy.

Blood Sugar: A Balancing Act
Anna was navigating life as a college freshman when she started to have unsettling symptoms. She recalls, “I noticed several changes, such as polyuria (excessive urination), excessive thirst and hunger, weight loss, severe headaches…changes in my skin, and constant illness.†As an 18-year-old student, Anna was left wondering what was happening to her body. Her roommate even joked with Anna about having diabetes. After checking online symptoms, Anna decided to schedule an appointment. She remembers, “After a visit to the health center they easily diagnosed me with Type 1 Diabetes. My WebMd self-diagnosis was correct for once!â€
The initial symptoms that Anna experienced were directly linked to the high levels of glucose, a type of sugar, accumulating in her bloodstream. This condition is called hyperglycemia (hyper = over/above, glycemic = related to glucose/sugar). In the short term, excess sugar is “locked out†of cells and is forced to stay in the bloodstream. Instead of being used for energy, the glucose builds up to dangerous levels in the blood.
When this buildup occurs, patients like Anna may suffer from headaches, fatigue, and extreme thirst. As the cells are starving for energy, the body may start to break down fat instead – a process which also produces acids called ketones. In extreme cases, too many ketones can cause dizziness, abdominal pain, or even coma.
The effects of high blood sugar explain Anna's symptoms, but what caused the hyperglycemia in the first place? The answer lies in a hormonal imbalance in Anna's endocrine system.
The Endocrine System
The endocrine system is made of diverse organs called endocrine glands located throughout the brain, throat, chest, and abdomen. These organs produce chemical messengers known as hormones, which travel through the bloodstream to control the major functions of the body. Most people are very familiar with the fight-or-flight hormone adrenaline as well as the multiple hormones that orchestrate puberty.
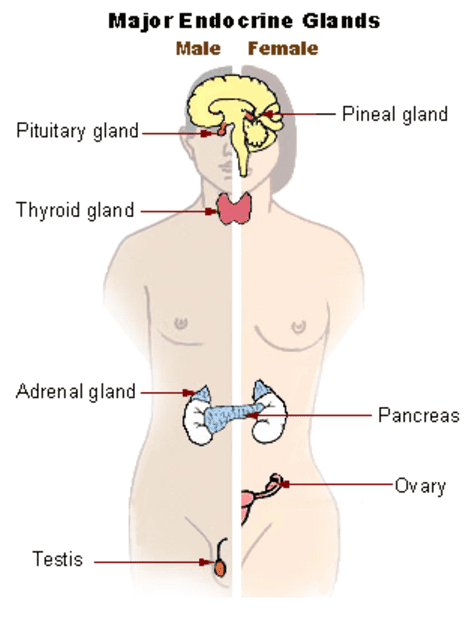
Hormones are also responsible for regulating blood sugar in the body. Although sugar is typically villainized as “unhealthy,†our bodies depend on a type of sugar called glucose to survive. After eating a meal rich in carbohydrates, our bodies break down the carbs into usable pieces – including glucose. Glucose then travels through the bloodstream to be converted into energy or stored for later use.
Unless a person has a medical condition such as diabetes, their body naturally works to regulate glucose levels in the blood. A gland called the pancreas monitors blood sugar levels and uses two major hormones to control glucose distribution: insulin and glucagon.
Insulin and Glucagon
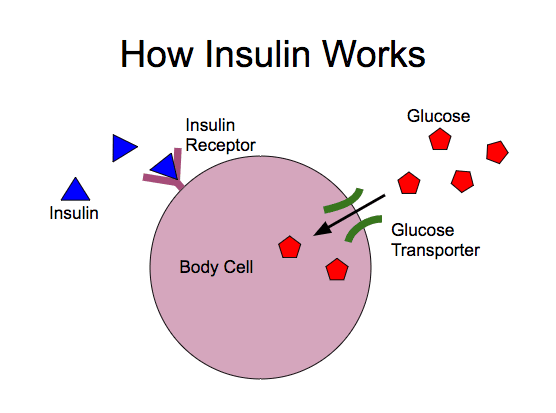
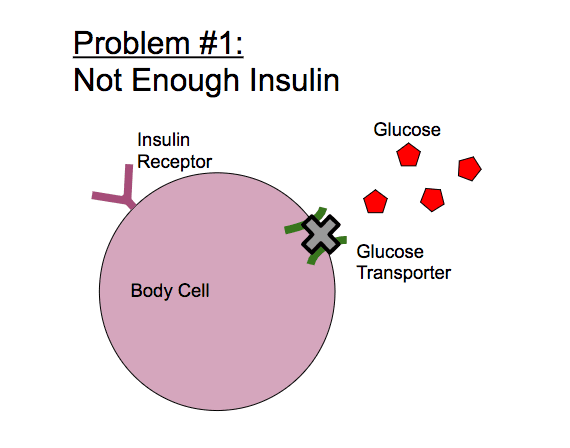
Insulin is produced when blood sugar levels are high, such as after a carbohydrate-rich meal. The pancreas pumps insulin into the bloodstream to help body cells absorb glucose molecules. Insulin acts as a “key†that “unlocks†body cells so that they can use glucose from the bloodstream for energy. Insulin also helps store excess glucose in liver and muscle cells to be used during times of low blood sugar.
When blood sugar is too low, (such as in between meals or during exercise), the pancreas releases a second hormone called glucagon into the bloodstream. Glucagon acts on the liver to release stored glucose and raise blood sugar. The pancreas can then produce more insulin to allow body cells to use the released glucose. Thus, insulin and glucagon work hand-in-hand to regulate blood sugar balance throughout the day and night.
Types of Diabetes
Diabetes stems from two types of problems. Type I is associated with insulin insufficiency while Type II is generally associated with insulin resistance.
As Meagan and Anna's bodies developed Type I diabetes, their pancreases became ineffective in regulating blood sugar. This inability to properly control glucose levels occurs in all people diagnosed with diabetes. Depending on a number of factors, doctors will categorize a patient's condition as a certain type of diabetes; though Type I and Type II are the most common types of diabetes, there are many others.
In general, Type I diabetes describes a condition in which the pancreas cannot produce enough insulin to regulate blood sugar. In many cases, the pancreas stops producing insulin altogether. Without sufficient insulin in the bloodstream, there aren't enough “keys†to let the glucose into cells. This condition is often diagnosed in childhood, but it also occurs in adults like Meagan and Anna. Nobody knows exactly what causes Type I diabetes, but genetics likely play a role.
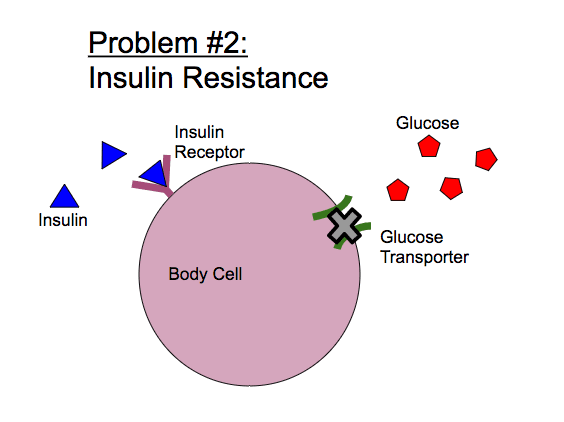
Type II diabetes is a condition in which the body cannot effectively use insulin to regulate blood sugar. Unlike Type I, It is typically diagnosed in adulthood. Type II occurs when insulin, the “key†to body cells, cannot properly open cells to let glucose inside. This phenomenon is known as insulin resistance, and it is due to a variety of interacting factors including genetics, environment, diet, and lifestyle. Each case is different, and scientists are still working to understand the root causes for this disease.
Like with other types of diabetes, Type II is usually diagnosed after a host of symptoms occur. Beth was 37 when she experienced “extreme fatigue and generally felt bad.†Blood work from her doctor revealed that her body had developed Type II diabetes. Beth – a devoted wife, mother, and active member of her church – was faced with the challenges of a chronic disease. The insulin that her pancreas produced wasn't properly unlocking the cells in her body, so they were not receiving the energy that they needed. At the same time, her unregulated blood sugar levels were putting her at risk. Under the supervision of her doctor, Beth soon started a treatment plan for her condition.
Long-Term Effects and Treatment Options
For all people diagnosed with diabetes, it's extremely important to see a doctor to avoid the long-term consequences of untreated hyperglycemia. The short-term symptoms are only the early warning signs of diabetes. If hyperglycemia remains unaddressed for many years, high blood sugar can contribute to the hardening of blood vessels. As blood vessels harden, blood flow is restricted. Complications can include heart problems, stroke, and significant foot problems due to lack of bloodflow. If patients produce no insulin at all (e.g. many patients with Type I diabetes), severe and life-threatening complications can occur if patients do not seek treatment.
Additionally, patients must avoid dangerously low blood sugar levels due to fluctuations in treatment and everyday life. In the case of a person with diabetes, severely low blood sugar can result from “over correcting†hyperglycemia during treatment. The symptoms of this condition, called hypoglycemia, range from mood changes to life-threatening issues. If the person has severely low blood sugar and does not receive glucose, they can become light-headed, fall unconscious, or even have a seizure. To avoid both hyperglycemia and hypoglycemia, each patient needs a comprehensive treatment plan including emergency preparedness.
Fortunately, patients have a large number of treatment strategies depending on their condition. Modern medicine has made diabetes quite manageable, and educational resources are widely available. Treatments will vary depending on the form of diabetes. For example, people with Type I diabetes must rely primarily on insulin because their pancreas does not produce enough (or any) insulin. For people with other forms of diabetes, multiple treatment options and combinations are available. All treatments are designed to keep blood sugar levels as close to normal as possible, and doctors will help patients choose a treatment plan using a variety of tools.

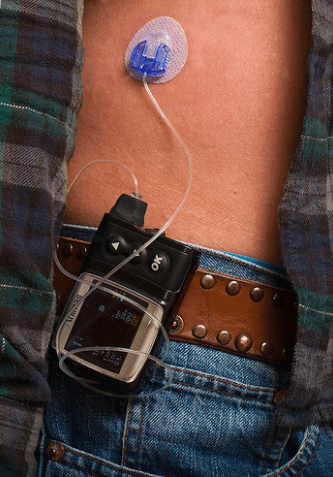
All treatment options are individualized, and they often change. Since diagnosis with Type I, Anna has switched from using insulin injections to an insulin pump. Still, she must be very conscious of her diet and activity in order to give herself the proper amount of insulin. “I am… more aware of my blood sugar changes for different types of workout[s],†said Anna. “Sometimes I need to adjust the amount of insulin I use depending on stress, sickness, exercise, etc.â€
Meagan also tried various treatments before finding a good plan for her. During pregnancy, Meagan took oral medication because her doctors believed that she had a certain type of diabetes called gestational diabetes, in which expectant mothers experience temporary blood sugar irregularities. The oral medication was prescribed to increase Meagan's sensitivity to insulin. After she gave birth, however, doctors realized that she had Type I diabetes. Meagan's body wasn't producing nearly enough insulin, so she was prescribed insulin pen injections. Meagan has since switched to using a pump and must balance insulin, physical activity, carbohydrates, and dosages everyday: “It's not a perfect science,†said Meagan. “I wish it was, but it's just not. It's not counting carbs and then just giving insulin.â€
Beth's treatment strategies for Type II diabetes have also changed over the years. In addition to diet modifications and increased exercise, she has used a combination of oral medications and insulin. One of Beth's former medications, called Actos, was taken off the market due to increased risk of bladder cancer and possible risk to the heart, liver, and other parts of the body. Beth has since switched to other oral medications, and she works diligently to integrate a consistent treatment plan into her family's busy lives.
With so many options and combinations of treatments, every person diagnosed with diabetes should develop a unique treatment plan. With the support of doctors, modern medicine, and discipline, many patients can be very successful in managing their condition.
.
(Source left- from Flickr, right- from Flickr)
What YOU Can Do!

⇛ Get Educated
If you have been diagnosed with diabetes, learn all you can.
To anyone who may already have been diagnosed, Beth advises: “Attend as many classes and trainings as you can. The more you know, the more in control you will feel.â€
If you have not been diagnosed, still learn all you can.
Educate yourself about lifestyle choices that can help lower your risk of certain types of diabetes such as Type II. Oftentimes, diet and exercise can greatly reduce your chances of developing diabetes. Get regular check-ups and ask your doctor about warning signs.
Education about diabetic crisis situations saves lives.
During daily life, people with diabetes can experience hypoglycemia when their blood sugar drops too low. This condition can be life threatening, but it can be treated with fast administration of sugar to the affected person.
As Anna pointed out, if more people were educated about diabetes, it would be easier to “recognize cases of severe hyperglycemia and hypoglycemia and respond to these health emergencies accordingly.†Knowing how to react in a crisis situation could save a life.
⇛ Get Connected
Connect with others to learn about diabetes and support those who have been diagnosed. Here are a few good places to start:
- Use the American Diabetes Association's website for educational resources and information to find local support groups.
- Take a look at Beyond Type I for support and education about Type I diabetes.
- Grab a free 12 month informational program from the American Diabetes Association.
- Check out Meagan's blog here.
There are millions of people who understand exactly what you are going through, and they will be your best support system. – Anna
⇛ Support, Support, Support!
Meagan stressed the importance of community and positivity during treatment. “I think if I were to say anything about diabetes, it is [this]: it takes a huge village and a lot of support and empathy and kindness for yourself,†she said.
Anna and Beth strongly echoed a need for support while they walk through this disease. Diabetes is challenging and scary, but love, understanding, and compassion for those who have been diagnosed is crucial.
Kindness, love, and support will make a world of difference!
About the author
 |
Amanda Piehler is an undergraduate at UGA double-majoring in Biology and Science Education. When she's not adventuring in academia, you can find her dancing, running, cooking, SCUBA diving, or hiding out in a local theatre. Connect with her on Facebook or email her at apiehler@uga.edu! More from Amanda Piehler. |