With only 50% of patients recovering fully in the long-term, anorexia is the deadliest psychiatric disorder. Typically associated with poor body-image and unhealthy eating habits, anorexia has captivated and bewildered the minds of laymen and scientists alike. While not every person suffering from anorexia is underweight, there is still a general misunderstanding of what is really going on in the mind and body. It is a myth that anorexia is a purely psychological phenomenon – where one's desire to be skinny goes too far. The reality of the disease is much more complex. With side effects ranging from osteoporosis and anemia to heart failure and nerve damage, the consequences are far more severe than just being “too skinny.â€
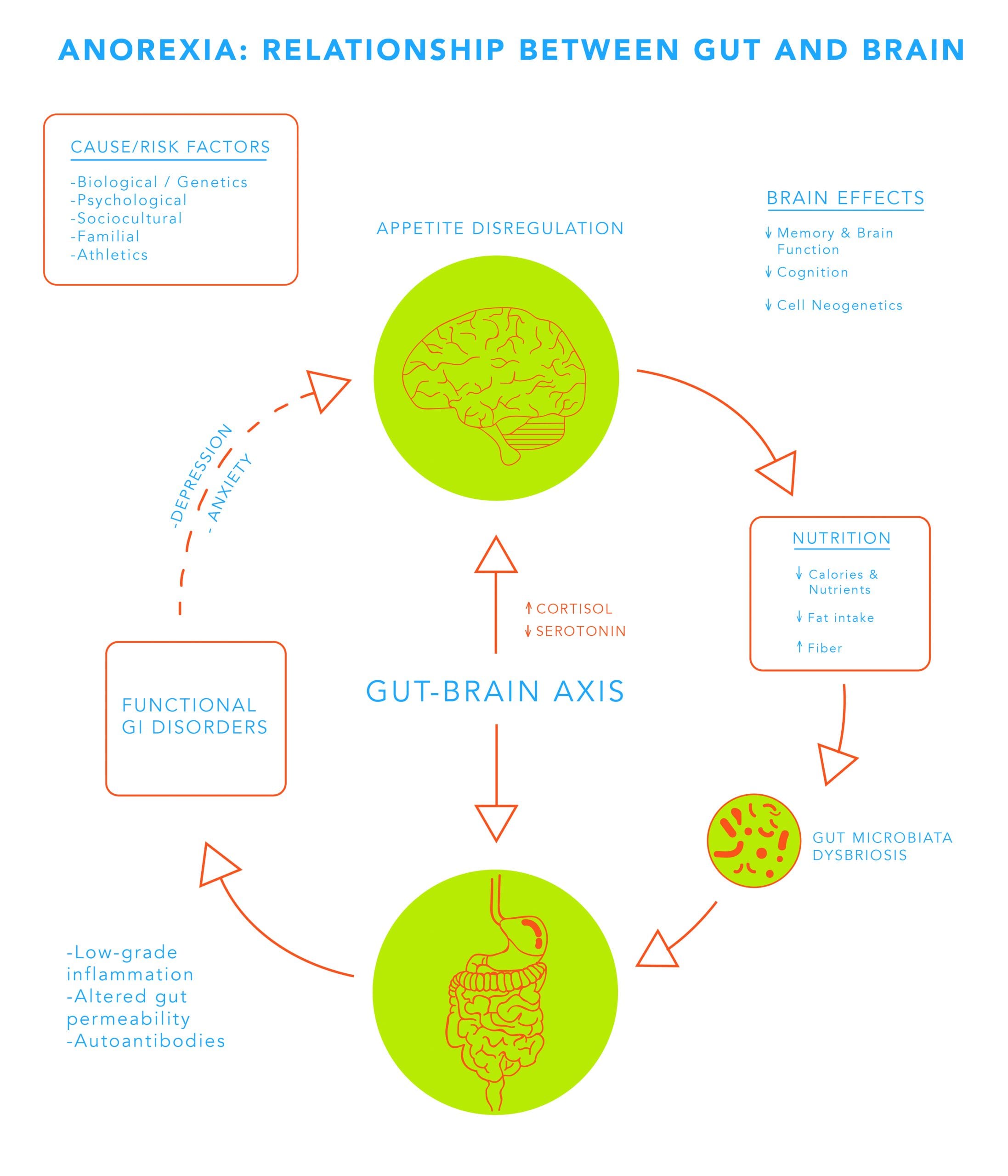
Anorexia typically “begins†with an environmental trigger, such as stress or a simple desire to eat healthier, that signals the desire to overexercise or restrict food intake. But not everyone who loses weight develops anorexia. Rather, some may have genetic predispositions – mentally, physically, or metabolically that drive habits that enforce anorexic behaviors. This results in typical anorexic habits such as increased drive for thinness, increased body dissatisfaction, and ongoing food restriction that perpetuates the cycle of behavior and reward, namely restricting food and losing weight.
This caloric restriction drives drastic changes in the gut microbiome, which is a collection of microorganisms in the GI tract that influences our metabolism and mood. While factors such as genetics, age, and sleep play a role in the diversity of microorganisms, fiber intake is a huge player in the gut's microbial composition and function.

What are the characteristics of the gut environment of anorexics? Chronic caloric restriction, food group imbalance, micronutrient deficiencies, and high fiber- to name a few. This results in dysbiosis, or microbial imbalance, that affects not only the host's metabolism, but behavior and the immune system as well. What was once a balanced and diverse environment now becomes competitive, selecting for microbiota that can sustain on low energy and nutrients.
Usually, our gut and brain communicate with each other via the “gut-brain axis†to let us know whether we are satiated or still hungry. Gut microbes can release chemicals, such as short-chain fatty acids (SCFAs) and hormones that affect the appetite and metabolism control centers of the brain. When we drastically reduce our food intake, our bodies get confused and the normal communication between the brain and the gut is impaired. A well-maintained intersection now becomes a traffic jam and unfortunately, that traffic jam seems to have lifelong effects for anorexics.
Our current “treatments†focus on refeeding and addressing psychosocial needs, but less so on fixing the microbial dysbiosis.
Knowing what we know now about the intricate connection between the gut and brain and its genetic underpinnings, it is important to translate this research to new therapies – such as prescribing pre/probiotics and the use of fecal-matter transplants. Studies have shown promising results by targeting the microbiota for treatment of many mood disorders, primarily by regulating serotonin levels, which has an active influence on appetite and behavior. Some bacterial strains have also been shown to alleviate symptoms of anxiety and stress-two hallmark symptoms of anorexia. These novel approaches could theoretically improve weight gain, decrease stress to the gut , and even reduce psychological symptoms!
While anorexia treatment has long focused on alleviating psychiatric symptoms, it is perhaps time to turn our attention to the relationship between the patient's gut and brain. The development of novel treatments that target the gut microbiome are essential if we are to properly tackle this disorder. All of these gut-brain factors, combined with the genetic effects on mental health and metabolism, might be of importance to improve long-term outcome of one of the most chronic psychiatric disorders of adolescence.
If you or someone you love are currently struggling with an eating disorder, contact the NEDA helpline (1-800-931-2237) for support, resources, and/or treatment options. You can also click to chat here.
About the author

Maria Flowers is an undergrad studying Biochemistry and Molecular Biology/Spanish at UGA. Her dreams are to continue demystifying the sciences through art and writing. In her free time, she loves to dance, read the New Yorker, write poetry, and listen to her favorite podcast “On Being” while doing yoga. She also loves frisson-ing to any and all types of music. If you wanna chat about science or her wide-array of special interests, you can email her at @ mwf38801@uga.edu.







